I am SO excited to share this guest post today! For the last year and a half, COVID has obviously been the most talked about topic pretty much everywhere. We have all heard of the numbers--how many have tested positive that day or which country is being hit the hardest, or what the death toll is. I feel very fortunate that nobody very close to me has had to be hospitalized due to COVID.
Something I've realized, though, is that because I don't see the effects with my own eyes, it's hard to truly understand the devastation it has caused--not just in the people who have survived COVID, but in the families who have lost people, the people who will have long-term complications, and especially the mental health of the front-line workers.
I haven't been inside of a hospital since before the pandemic so I have no idea just what it looks like and how it's changed. When I started this COVID Diaries series, I really hoped I'd be able to hear from someone that works closely with COVID patients. I wanted to hear the "realness" of what is happening and not just see the numbers on the news. I wanted to be able to know what it actually involves and what the full process is.
Interestingly, the guest post that answers a lot of my questions is written by none other than my very own sister! She lives in Illinois, so I don't see her nearly as often as I'd like, but I was thrilled when she said she'd like to write this post.
There are a couple of things I want to point out before I turn it over to her:
1) This is not a political post and I do not want to bring politics into it at all. Nor do I want to turn this into a debate about whether to vaccinate or not. Normally, I publish every comment that is written on my blog (minus the spam) but I won't be publishing political comments here. This is just a post of my sister's experience of what she sees and deals with every workday and I'm grateful to her for sharing her thoughts.
2) This is written following all HIPAA laws--my sister doesn't use any identifying information or photos. She takes that very seriously. (The photos that show the different types of oxygen masks can be found online; I've linked to the sources. They are not my sister's photos).
Okay, enough from me. Introducing my sister, Jeanie...
My name Jeanie and I am Katie’s sister. I work as an occupational therapist at a level 1 trauma hospital. I am writing this guest post in the hope of giving insight as to what it is like to work in a hospital during the COVID-19 pandemic. As a disclaimer, nothing I am writing has anything to do with politics or my own personal beliefs. Everything I will include in this post is what I see with my own eyes in this occupation.
I am confident in saying that many healthcare workers are completely fed-up with reading inaccurate information on social media from people who have no affiliation with the medical or science field but continue to re-post this misleading information. (I could make that into a whole post by itself, but I will stop there).
If you are not familiar with an occupational therapist, an OT can work in several different settings: homes, schools, outpatient clinics, mental health centers, hospitals, etc). Personally, I think the word ‘occupational’ should be changed to ‘functional’. We should be called Functional Therapists because our goal is to help patients return to their daily lives: dressing and feeding themselves, writing their names, dialing a phone, opening medication bottles, managing their oxygen cords while walking, etc.
As an OT in the hospital, the job details can change drastically depending on which unit I am working. Occupational therapists and physical therapists work together with patients in a lot of situations. If I am in the intensive care unit (ICU) and the patient is on a ventilator, we (the PT and I) may just be working with a patient on balance/tolerance to sit upright—the eventual goal being that the patient will be able to sit up and wash their face, for example.
Or if I am working on the orthopedic floor, then I may be teaching someone how to use long-handled tools so they can dress themselves without bending over after having a hip replacement.
A big part of my job at the hospital is to help determine where the patient should go once they are ready to the leave the hospital. Are they safe to go home? Do they need home care? Do they need intensive rehab at a facility? Do they need long term care? The rest of the medical team relies on the therapists for the appropriate recommendations. (This causes a lot of stress because you want to make the correct decisions.)
For COVID-19 patients there is a spectrum of care:
The most critical is the ICU (intensive care unit). From there, it goes down to step-down ICU (SDICU). Then there is the cardiac floor or general floor (depending on the severity of the illness).
General Floor
From what I have seen, patients on the general floor may or may not have been vaccinated for COVID-19 (most are unvaccinated; some are vaccinated but are overdue for a booster shot). The patients on the general floor are on a low amount of supplemental oxygen, usually no more than 6L (liters).
These patients can typically tolerate some daily activities. (As a frame of reference, people on oxygen at home are usually on 2-4L.) When I work with these patients, I usually teach them energy conservation strategies (moving slowly, pacing oneself, pursed-lip breathing techniques) and how to incorporate those into daily tasks.
For example, I may educate the patient on how to take a shower without becoming completing exhausted: using a shower chair; keeping the bathroom door open and overhead fan on to circulate air; keep the oxygen flowing during the shower; cross legs to wash feet or use a long handled sponge to avoid bending forward; and other things like that.
Once the patient is educated, I will have them complete the task while I monitor their incorporation of what was taught. I also keep an eye on their vital signs before and after the shower and monitor them for any signs of inability to tolerate the activity. Many patients are VERY happy to finally take a shower but also are grateful for strategies that will help them at home.
Cardiac floor
Covid patients on the cardiac floor are typically more ill and have increased oxygen needs due to COVID pneumonia (this is where sacs in the lungs fill with fluid, limiting the ability to take in oxygen).
Many of these patients also develop additional medical issues. It is not uncommon for COVID patients to develop blood clots or pulmonary embolisms (PE) or even to have a stroke. So these patients present with COVID and now also have a PE; or have COVID and now have a new stroke.
The therapy for these patients varies greatly. Some can only tolerate seated exercises in a chair; some work on energy conservation techniques with daily activities; some learn to manage an oxygen cord while walking with a walker (these patients will likely be able to go home now with oxygen).
It is more challenging to treat patients who have COVID and subsequently had a stroke. The amount of personal protective equipment the staff wears in the room becomes very warm, very quickly. Physically assisting patients to sit up on the edge of the bed or transfer to a chair will leave the therapist(s) sweating. A lot of times, these patients are on a blood thinner medication and want the thermostat all the way up, making it even warmer in the room.
Step-Down Intensive Care Unit (SDICU)
Most of our patients on step-down intensive care unit (SDICU) have severe COVID pneumonia and are on heated high flow oxygen (HHF) or on a BiPap machine to help them breathe.
While the patients on the general floor are on 6L or less of oxygen, the patients on SDICU are on typically anywhere from 8L to 40-60L of oxygen, depending on the oxygen levels in their blood. The oxygen meter hooked up to the wall (like you see in a doctors office) goes up to 15L.
If the patient requires more oxygen than that, they go on the HHF or BiPap. These machines allow a higher liter-per-minute delivery rate as well as the ability to change the percentage of oxygen delivered. I will try and keep this simple but the lowest level to highest level of oxygen looks like this: (Note: these are not photos of my sister's patients; I've linked the sources to the photos below them)
1. Room air (no oxygen required)
2. On a regular nasal cannula hooked up to the wall (up to 15L). This is just the tube that you see people at home with—where it delivers oxygen into your nostrils.
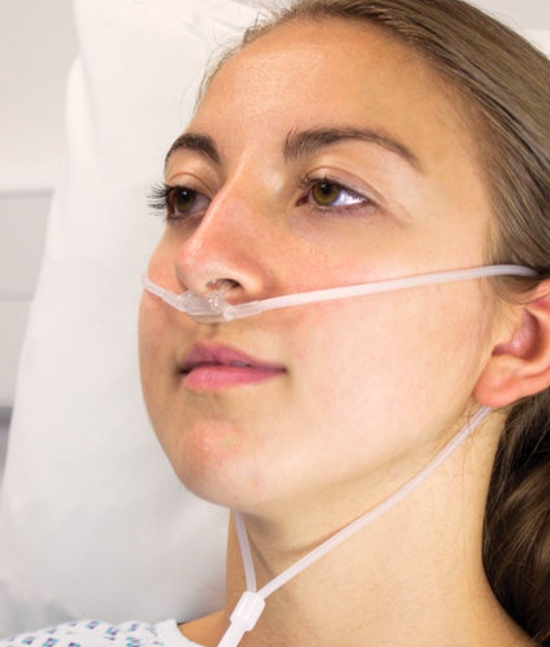 |
| Photo of a nasal cannula - source |
3. On heated high flow (up to 60L, 100% oxygen) given through a special high-flow machine and special nasal cannula that can deliver that amount of oxygen. These patients are in the SDICU.
 |
| Photo of a heated high-flow oxygen machine - photo source |
4. BiPap. This is a mask that has velcro straps that tightens the mask over the nose and mouth and uses high pressure to force the air into the lungs. Patients find it to be very uncomfortable because the amount of pressure needed feels extreme. These patients are in the SDICU.
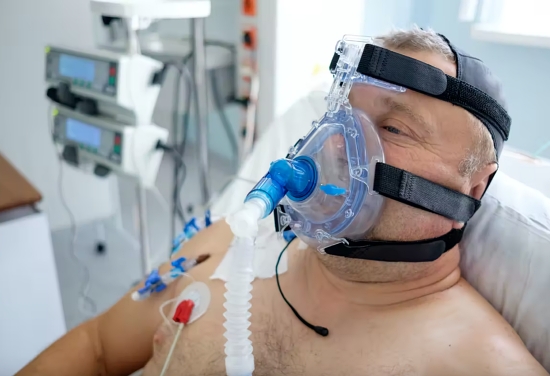 |
| Photo of a BiPap machine - source |
5. If the patient can’t keep the oxygen levels up with BiPap, the only step left is to be on a ventilator. This is a machine that does the breathing for the patient. These patients are in the ICU where the main goal is survival.
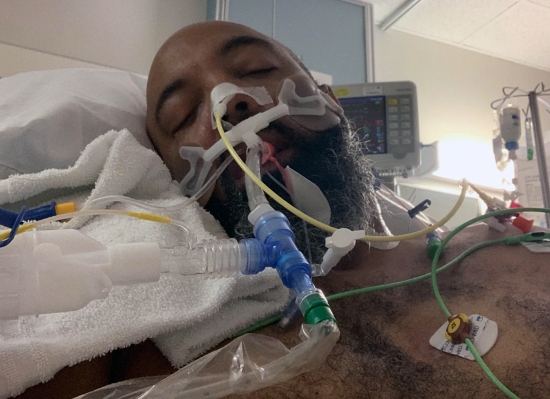 |
| Ventilator - photo source (this is a great article to read!) |
 |
| Tracheostomy (a surgical hole in the throat) for a ventilator; used for long-term vents |
Treating patients in the SDICU is extremely tricky. The main goal is to keep their blood oxygen levels up. (For reference, a healthy oxygen is about 95-100%.) These patients’ oxygen levels tend to drop very quickly with any movement.
It is not uncommon to go into a room and the patient has oxygen levels of 92% when they are on their stomach. Lying on their belly (called ‘proning’) is encouraged because it has been shown to help improve oxygen levels. But if they roll over, stand up, or get onto the commode, etc. their oxygen may drop into the 70s (or even 60s) very quickly. This is scary because it tends to take a long time for COVID patients’ oxygen levels to come back up.
This is why we encourage patients to use pursed-lip breathing (breathe in through the nose and blow out the mouth), move very slowly, and take rest breaks instead of rushing though the activity (which may just be getting up from the chair). If the patients’ oxygen levels do not come back up into the high 80s or low 90s, then we usually have to give the patient more oxygen to help with that.
I treated a woman who was in the SDICU and was on 8L of oxygen. Her oxygen levels were 94% in bed. She needed to use the toilet, and just by getting up to the commode, her oxygen levels dropped to the 70s. Over the course of 13 minutes, I gradually increased her oxygen to 15L. Her oxygen level was still only in the mid 80s. At this point, she had to go back on the heated high flow machine or prone in bed to get the numbers back up. (This patient laid face-down and the numbers did come back up).
These patients are usually (and understandably) anxious—some say they feel like they are drowning, or that they can’t get a good breath. They either want to see the monitor so they can see what their numbers are, or some ask that the monitor be turned away and alarms turned off because knowing the numbers increases their anxiety.
As a therapist, we are trying to prevent the patient’s body from becoming de-conditioned during long-term hospitalization (when your body is lying in a bed for so long, it becomes difficult to move and function as you did previously); prevent bed sores by having them change positions; improve digestion and prevent constipation by having them sit up for meals; and help improve circulation to prevent blood clots.
However, we also know these patients have a hard time maintaining good oxygen saturations (like I said, it can change very quickly) and we don’t want to “push” the patient because if their numbers stay low, they may have to change from nasal cannula to high-flow or high-flow to BiPap. We use extreme caution when a patient is on BiPap because the only step left is intubation if the oxygen levels don’t stay up.
These patients cannot tolerate much activity and even if the patient is physically able to walk in the room, the machines (HHF and BiPap) have limited cords/tubing; this prevents us from helping the patient walk any distance. They can usually walk a few feet forward/back within the range of tubing.
As the OT, I may work on simple arm/leg exercises; or bathing/grooming in attempts to get the patient to improve their endurance by participating in simple tasks.
Intensive Care Unit
When worse comes to worst, if patients are not able to maintain their oxygen levels on BiPap, then the only step left is being put on a ventilator. Some patients (or family members who have power of attorney) choose to refuse the ventilator, even though they know the outcome will be death.
This is a horrible horrible situation for families and is a strong reason why people should have a discussion with loved ones about what their wishes are if they are ever in this situation (not just with COVID, but with any situation that may arise).
It is not uncommon for many of the vented patients to end up needing a feeding tube and a tracheostomy (a hole in the throat) which is then hooked up to the ventilator. Many vented patients go into multiple organ failure and may require continuous dialysis at the bedside.
Once a COVID patient is in ICU on a ventilator, I don’t see them for therapy. They are usually prone for up to 18 hours a day and the goals of care are focused on patient survival.
Occasionally, I will help the medical team “prone someone”. This usually requires 4-5 staff members at once—one needs to be the respiratory therapist, who manages the ventilator tubing coming from the patient’s mouth, and rest of the team forms a type of “cocoon” around the patient with two bedsheets. On a specific count, everyone works in synchrony to roll the patient onto or off of their belly.
It sounds simple, but remember… you are managing multiple IVs, a central line, a foley catheter, vent tubing etc. Also, some of the patients are very heavy, which further complicates the process.
If the patient continues to decline once they are on the ventilator, the palliative team will usually talk to the family to give them insight into what the prognosis is and what the options are moving forward (tracheostomy for ventilation, feeding tube, dialysis).
Many families chose to withdraw care from their loved one when they realize survival is unlikely and it will cause undo suffering if they continue aggressive care. Withdrawal of care is common if a patient is on BiPap but still unable to keep the oxygen levels up and has noticeable labored breathing, agitation, etc., and it has been determined through the patient and/or family that they do not want intubation.
At my hospital, families are allowed to visit for end of life (some are allowed in the room and some are not, depending on various factors). The nurse explains to the family what to expect when they withdraw care, and when the family is ready, the nurse will administer medications to help keep the patient comfortable before withdrawing the BiPap (or ventilator). At that point, most COVID patients pass away very quickly because their body has been fighting shutting down for some time.
I had a patient who did not want to be intubated but was agreeable to BiPap (this is not uncommon). The patient “fought” for his life and I remember hearing him beg his nurse “please don’t let me die”. The nurse responded, “I am going to do everything I can to help you survive”.
Days later, the patient was in obvious respiratory distress and the family came up to the hospital. I brought them chairs so they could sit outside of his room (which had a glass wall) to see him before the nurse withdrew care (per family request). He passed away within 10 minutes.
My heart was broken for the patient and his family, but also broken for the nurses who do this day-in and day-out. For an ICU nurse, withdrawing care is not unheard of; however, I am sure they never expected to have to withdraw care on so many patients in such a short period of time.
When a patient is able to maintain a good oxygen level, and they are able to come off of the ventilator, then therapy will start again. These patients are extremely weak and usually require 2-3 people just to sit up on the edge of the bed.
They typically now go in reverse order for oxygen (they were on the vent, then move to BiPap, then to HHF, then nasal cannula). The physical therapist and occupational therapist work together with these patients as treatment is directed by what the patient can handle without overdoing it.
These patients usually will not go directly home from the hospital, but will go to a long-term care facility that works on lowering their oxygen needs (patients are not discharged home when they are on BiPap or heated high flow). If the patient improves at long-term care and has lower oxygen needs, they may then go to a different facility where the focus is more on getting stronger.
All of this is a very long process. It is not uncommon to have patients in SDICU and/or ICU for 4-8 weeks.
A few other things… All patients entering the emergency room have a rapid COVID test done and then have a PCR test (which is more accurate but takes longer) performed as well. If the rapid test is negative, then the patient is not put into COVID isolation, unless COVID is still suspected based on patients’ symptoms. If the rapid test is positive, then the patient is put in COVID isolation. Occasionally, we have someone who has a negative rapid test only to find out the PCR test is positive. PCR tests take about 24 hours to get back (much better than the 10-11 day wait time when COVID first started).
COVID isolation requires staff to wear a gown, gloves, an N95 respirator (or CAPR) with a surgical mask over it, and a face shield.
 |
| Kelly (the physical therapist) and Jeanie dressed to help a COVID patient sit up |
One significant challenge is that patients cannot hear you through the masks, especially if the patient is elderly and/or relies on reading lips. If a non-COVID patient is hard of hearing, I typically bring my phone into the room and use “voice to text” in my phone’s note pad to allow easy/fast communication without having to write everything down. So I can say into my phone “My name is Jeanie and I am from therapy. I am here to help you get stronger. Would you like to get up to the chair this morning?”
Then the patient can read it and we can get moving. However, I can’t bring my phone into a COVID patient’s room, so communication is huge barrier, especially if the patient does not speak English. We have a speaker phone in the room to allow access to an interpreter. But the interpreter also has difficulty understanding us through the masks and the whole process is a shit show. (Just FYI, I NEVER use my phone for ANY personal medical information about a patient; it is just for general directions and communication).
Another big challenge is making sure you bring everything you are going to need for your treatment in the COVID room the first time you enter. I usually put on my N95, surgical mask and face shield, then I crack the door and ask the patient if there is anything they need (water, Kleenex, etc) before I come in. If the patient can hear me, I gather whatever they request.
Once I am in the room, it is quite the ordeal if I forgot something. I can either press the call light and wait for someone to bring me what I need or I can take all of my personal protective equipment off, go get the supplies, put all the PPE on again and then finish my treatment.
The easiest way is obviously to use the call light; but many of the staff members who answer call lights are also in isolation rooms. (We had 14 COVID patients out of 26 in one unit last Sunday). And some patients “add on” what they want once I get into the room. I had to have a nurse aide come to the room I was in three times on Sunday because the patient asked for water, which was brought to the room. Once it was there, they decided they did not want ice water but plain water. Then they wanted extra Kleenex. And then they wanted a brush, not a comb.
Now, I do understand these are all normal requests. In a non-isolation room this is no big deal. In a COVID room, all of this takes time.
I bring up time because this is also a factor I wish more people understood. It is not uncommon to go into a room and someone is talking on their phone. To me, the appropriate response from the patient should be to tell their caller “A staff member just came in, let me call you back shortly”.
It’s extremely frustrating to the staff just how many patients (not just COVID patients) continue their conversation as if you never walked in the room. The younger generation likes to FaceTime and some will stay on FaceTime even while you are trying to talk to them. Some patients will answer the phone in the middle of the session and begin a long-winded conversation with someone.
This is taking up a staff member’s time that could be spent with another patient. Yes, we can take off all the PPE, leave the room, go see someone else and come back (and we do at times). But this is a general waste of time and PPE. (I do understand there are occasional important calls; I am not referring to those).
Some of these patients who were on their phones then complain that it took “…20 minutes to get some water” or “I waited a long time for someone to answer my call light” don’t see the irony that they are a contributing factor as to why there is a delay in “instant” service.
A big issue that came along with the COVID pandemic is bed availability. Working at a level 1 trauma hospital means that we treat acute strokes, multiple traumas from accidents, spinal cord injuries, brain injuries, victims of violent crime, open-heart surgery patients, etc. I say this because most of these patients need an ICU bed.
However, many of ICU beds are occupied by COVID patients on ventilators, which means the turn-over time for a bed can be weeks. It can be difficult to find a long-term care facility to take a COVID patient once they are medically stable for discharge because the long-term care facilities are also full of “long COVID” patients (whose symptoms last for months after acute COVID) and do not have bed availability.
Patients become frustrated that they have to wait in the “overflow” area of the emergency room for a few days waiting for a room upstairs. (Just to clarify, the patient is NOT in the waiting room of the ER; they have a regular hospital bed, but they are just not on the medical floor).
Well, the reason for the slow bed turnover is because long-term care facilities are likely full; and rehab facilities, if they aren’t full already, want a patient to wait 10-14 days after a positive test before transferring. There are also family members who do not want to or cannot provide increased care for their loved one after discharge so those patients are also waiting on placement.
Medical insurance is another frustrating component—many insurances do not approve rehab when it is needed and this can take days and days to resolve. So at any given time, there are multiple patients ready for discharge but there is no where to send them and this creates a back up.
The Mental and Emotional Toll
I have met a patient who continued to say “COVID is not real” despite the fact that he was on BiPap due to COVID. He did not survive.
I have met patients who came to the hospital for help but declined the medications being offered (which they have a right to do). They did not survive.
I have met a patient who was unvaccinated and both she and her spouse were hospitalized. The first thing she asked me was, “When can I get vaccinated?” She told me her spouse was “down the hall” and they “both had COVID”. Her spouse declined overnight and was not down the hall, but in SDICU. He did not survive. They had been enjoying retirement while traveling south in the winter, north in the summer. She is alone now.
The crazy thing is that so many of these patients were not anywhere near dying when they got COVID. They were working, productive members of society. Or they were enjoying retirement with their spouse and their grandchildren. They may been otherwise healthy, or they may have had some minor medical issues (like everyone does when they get older—but certainly not something that put that patient near death before getting sick.).
I treated a younger lady who lost her spouse to COVID after she herself was hospitalized with COVID. This woman was so put together—she wore nice nail polish and had a very friendly demeanor (she reminded me of my cousin). I remember getting her up to the chair and she wanted her picture taken to send to her children. She gave a thumbs up and I snapped a photo with her camera. She immediately sent it to her children.
Her health declined rapidly. And when it came to it, she declined intubation. I often think of her and her spouse together again in eternity; her children left parentless over just a few days.
Those are cases you just can’t forget.
Being unvaccinated definitely puts someone in a higher risk category (I can say with confidence that probably 90% of our SDICU and ICU patients are unvaccinated). Also, obesity puts people at a higher risk.
Not all of these patients die. Some go on to long-term care. Some eventually make it to a rehab facility. I also work at a rehab facility a few days a month, and I see these COVID patients months after their original hospitalization. These are patients who are in the “survived” COVID category, but most people never realize the road that patient has traveled to get to that point in rehab, or that they may never go back to their pre-COVID life due to the long-term side effects from COVID.
But that is a whole different post… “long covid”. I had a patient who was hospitalized in the spring 2021 for 7 weeks with COVID. She made it to a long-term care facility and got off the vent. I saw her back at our hospital in the fall for complications. She has been back and forth from LTC to the hospital for seven months; she has still not been home and requires assistance for every daily task.
It’s not just about the death numbers in reference to COVID—there is a huge area in between the “recovered or died” categories that nobody talks about.
Like most healthcare workers, I am grateful for the opportunity to help these patients. But to say we are tired is an understatement. Pray for your medical team—not only for their physical health but for the mental strain they are under. Be kind. Be patient if you go to the hospital. They are doing their best.
I will leave you with a personal thought that I have often shared with patients (even before COVID). At some point, patients are responsible for their own health. You cannot rely on the doctors and hospital staff to “fix” things if you are not doing your part.
For example, if you have diabetes and have been educated on eating habits, exercise habits, checking your blood sugar daily, and taking your insulin as prescribed but you still choose to not do these things, that is on you. Yes, the doctors can help you out of a critical situation, but you also have a responsibility to take care of yourself.
It’s similar with being overweight. Or with smoking. Or using drugs. Et cetera. We all have some control over our health. There are factors we can’t control (our age, sex, genetics) but there are factors we CAN control. I encourage everyone to do what they can to take control of their own health!
(This is a guest post as part of my COVID Diaries series. You can read more about that and what I'm looking for here. If COVID has affected your life/job in a huge way, I'd love to hear from you!)



























